November 26, 2019
Why Clinical Trials are Important
I’m positive you’ve heard the term before. “Clinical trial” is that magical combination of words used as a descriptor in a whole slew of daytime TV commercials for products like actual FDA-approved prescription medications to over-the-counter deodorants. Some sneaky manufacturers like to slip in the word “clinical” to seem like legitimate consumer advocate groups and government regulations have already looked at the product and gave it a pass. This is not always true. But what does that term even mean? Should we automatically be more trusting as consumers when packaging or bubbly commercial promises clinical testing? Let’s take a look.
 When it comes to clinical research there are actually two types that manufacturers and researchers perform: clinical trials and observational studies. According to the National Institute on Aging, observational studies “observe people in normal settings. Researchers gather information, group volunteers according to broad characteristics, and compare changes over time. For example, researchers may collect data through medical exams, tests, or questionnaires about a group of older adults over time to learn more about the effects of different lifestyles on cognitive health. These studies may help identify new possibilities for clinical trials.” On the other hand, clinical trials “are research studies performed in people that are aimed at evaluating a medical, surgical, or behavioral intervention. They are the primary way that researchers find out if a new treatment, like a new drug or diet or medical device (for example, a pacemaker) is safe and effective in people. Often a clinical trial is used to learn if a new treatment is more effective and/or has less harmful side effects than the standard treatment.” Clinical trials are often used in drug development and are sometimes described by phase which is defined by the U.S. Food and Drug Administration.
When it comes to clinical research there are actually two types that manufacturers and researchers perform: clinical trials and observational studies. According to the National Institute on Aging, observational studies “observe people in normal settings. Researchers gather information, group volunteers according to broad characteristics, and compare changes over time. For example, researchers may collect data through medical exams, tests, or questionnaires about a group of older adults over time to learn more about the effects of different lifestyles on cognitive health. These studies may help identify new possibilities for clinical trials.” On the other hand, clinical trials “are research studies performed in people that are aimed at evaluating a medical, surgical, or behavioral intervention. They are the primary way that researchers find out if a new treatment, like a new drug or diet or medical device (for example, a pacemaker) is safe and effective in people. Often a clinical trial is used to learn if a new treatment is more effective and/or has less harmful side effects than the standard treatment.” Clinical trials are often used in drug development and are sometimes described by phase which is defined by the U.S. Food and Drug Administration.
 So, why go through the trials (pun intended) and tribulations of rigorously comparison testing medicinal practices and products? It’s a complicated question, and may largely depend on who you ask: researchers or patients. Researchers find that clinical trials can only add to benefit scientific and medical research as more data means more information to learn and develop from. As for patients and patient advocacy groups, participating in clinical trials have offered some confidence and control over their illness, while others feel taken advantage of and used as an experiment. This is largely dependent on the success of the trial. Regardless of opinion on clinical trials, they are accepted as important for discovering new treatments for diseases, as well as new ways to detect, diagnose, and reduce the chance of developing the disease.
So, why go through the trials (pun intended) and tribulations of rigorously comparison testing medicinal practices and products? It’s a complicated question, and may largely depend on who you ask: researchers or patients. Researchers find that clinical trials can only add to benefit scientific and medical research as more data means more information to learn and develop from. As for patients and patient advocacy groups, participating in clinical trials have offered some confidence and control over their illness, while others feel taken advantage of and used as an experiment. This is largely dependent on the success of the trial. Regardless of opinion on clinical trials, they are accepted as important for discovering new treatments for diseases, as well as new ways to detect, diagnose, and reduce the chance of developing the disease.
 Revive® is a new, FDA-approved, reusable bladder support device designed for women suffering from light bladder leaks as a result of Stress Urinary Incontinence or SUI. SUI is the involuntary loss of urine whenever the bladder, urinary tract, or abdomen is put under slight pressure through activity. Activities like running, coughing, or laughing may trigger these leaks in people with SUI. Revive® was designed to fit and move with women’s anatomy and internally support the urinary tract for up to 12 hours a day of leak protection. Clinical trials of Revive found that:
Revive® is a new, FDA-approved, reusable bladder support device designed for women suffering from light bladder leaks as a result of Stress Urinary Incontinence or SUI. SUI is the involuntary loss of urine whenever the bladder, urinary tract, or abdomen is put under slight pressure through activity. Activities like running, coughing, or laughing may trigger these leaks in people with SUI. Revive® was designed to fit and move with women’s anatomy and internally support the urinary tract for up to 12 hours a day of leak protection. Clinical trials of Revive found that:

What is a Clinical Trial?
 When it comes to clinical research there are actually two types that manufacturers and researchers perform: clinical trials and observational studies. According to the National Institute on Aging, observational studies “observe people in normal settings. Researchers gather information, group volunteers according to broad characteristics, and compare changes over time. For example, researchers may collect data through medical exams, tests, or questionnaires about a group of older adults over time to learn more about the effects of different lifestyles on cognitive health. These studies may help identify new possibilities for clinical trials.” On the other hand, clinical trials “are research studies performed in people that are aimed at evaluating a medical, surgical, or behavioral intervention. They are the primary way that researchers find out if a new treatment, like a new drug or diet or medical device (for example, a pacemaker) is safe and effective in people. Often a clinical trial is used to learn if a new treatment is more effective and/or has less harmful side effects than the standard treatment.” Clinical trials are often used in drug development and are sometimes described by phase which is defined by the U.S. Food and Drug Administration.
When it comes to clinical research there are actually two types that manufacturers and researchers perform: clinical trials and observational studies. According to the National Institute on Aging, observational studies “observe people in normal settings. Researchers gather information, group volunteers according to broad characteristics, and compare changes over time. For example, researchers may collect data through medical exams, tests, or questionnaires about a group of older adults over time to learn more about the effects of different lifestyles on cognitive health. These studies may help identify new possibilities for clinical trials.” On the other hand, clinical trials “are research studies performed in people that are aimed at evaluating a medical, surgical, or behavioral intervention. They are the primary way that researchers find out if a new treatment, like a new drug or diet or medical device (for example, a pacemaker) is safe and effective in people. Often a clinical trial is used to learn if a new treatment is more effective and/or has less harmful side effects than the standard treatment.” Clinical trials are often used in drug development and are sometimes described by phase which is defined by the U.S. Food and Drug Administration.
Clinical Trial Landmarks
Like most modern advancements in medicine, clinical trials got their start centuries ago, and have grown and advanced to the clinical trials we know and trust today. Here is a brief history of the notable advancements in the clinical trial: 562 BC - 1537: Clinical trials can be found in the bible, not performed by a medic, but a king. The scripture records that King Nebuchadnezzar, who was a fierce military leader, had wanted his constituents to eat meat to keep them healthy. In light of legume fans protesting, the king offered that they may eat the legumes and water for 10 days. When he saw that those who ate vegetables were healthier than meat-eaters, he let them continue their diet. 1747: James Lind and Scurvy Trial: James Lind is noted as being the “father of the clinical trial”, with his test that was conducted aboard a ship that was full of sailors with scurvy. He took 12 men with similar symptoms and diet and broke them up into treatment groups - “Two were ordered each a quart of cyder a day. Two others took twenty-five drops of elixir vitriol three times a day … Two others took two spoonfuls of vinegar three times a day … Two of the worst patients were put on a course of sea-water … Two others had each two oranges and one lemon given them every day … The two remaining patients, took … an electary recommended by a hospital surgeon.” Although Lind ran these trials, it would be years before citrus fruits were used as a way to combat scurvy as they were very expensive at the time. 1800: Arrival of Placebo: While the term “placebo” first appeared in medical literature in 1811, it was not used in practice as we know it in modern terms until 1863 when Austin Flint planned the first clinical study. He compared an herbal remedy to a known treatment for 13 patients suffering from rheumatism. The result was using the herbal remedy to improve overall confidence in patients that their ailments were subsiding. While our modern version of clinical trials are conducted much differently than in the 16th century, there is no doubt of humans’ need to test and compare results in clinical settings for various practices and drugs.Why We Need Clinical Trials
 So, why go through the trials (pun intended) and tribulations of rigorously comparison testing medicinal practices and products? It’s a complicated question, and may largely depend on who you ask: researchers or patients. Researchers find that clinical trials can only add to benefit scientific and medical research as more data means more information to learn and develop from. As for patients and patient advocacy groups, participating in clinical trials have offered some confidence and control over their illness, while others feel taken advantage of and used as an experiment. This is largely dependent on the success of the trial. Regardless of opinion on clinical trials, they are accepted as important for discovering new treatments for diseases, as well as new ways to detect, diagnose, and reduce the chance of developing the disease.
So, why go through the trials (pun intended) and tribulations of rigorously comparison testing medicinal practices and products? It’s a complicated question, and may largely depend on who you ask: researchers or patients. Researchers find that clinical trials can only add to benefit scientific and medical research as more data means more information to learn and develop from. As for patients and patient advocacy groups, participating in clinical trials have offered some confidence and control over their illness, while others feel taken advantage of and used as an experiment. This is largely dependent on the success of the trial. Regardless of opinion on clinical trials, they are accepted as important for discovering new treatments for diseases, as well as new ways to detect, diagnose, and reduce the chance of developing the disease.
Revive® & Clinical Trials
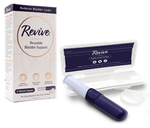
 Revive® is a new, FDA-approved, reusable bladder support device designed for women suffering from light bladder leaks as a result of Stress Urinary Incontinence or SUI. SUI is the involuntary loss of urine whenever the bladder, urinary tract, or abdomen is put under slight pressure through activity. Activities like running, coughing, or laughing may trigger these leaks in people with SUI. Revive® was designed to fit and move with women’s anatomy and internally support the urinary tract for up to 12 hours a day of leak protection. Clinical trials of Revive found that:
Revive® is a new, FDA-approved, reusable bladder support device designed for women suffering from light bladder leaks as a result of Stress Urinary Incontinence or SUI. SUI is the involuntary loss of urine whenever the bladder, urinary tract, or abdomen is put under slight pressure through activity. Activities like running, coughing, or laughing may trigger these leaks in people with SUI. Revive® was designed to fit and move with women’s anatomy and internally support the urinary tract for up to 12 hours a day of leak protection. Clinical trials of Revive found that:
- 71% of women experienced a reduction in SUI symptoms
- 75% of the time women felt dry while using Revive®
- 83% of users would recommend to others
- 90% of participants felt the product was a good fit upon first use